Most people think of arthritis as a knee or hand problem. Achy fingers, stiff hips, swollen joints you can see. But autoimmune arthritis doesn’t really follow neat rules. It can show up in places you don’t expect, including the jaw. And when it does, eating, talking, even yawning can suddenly feel like work.
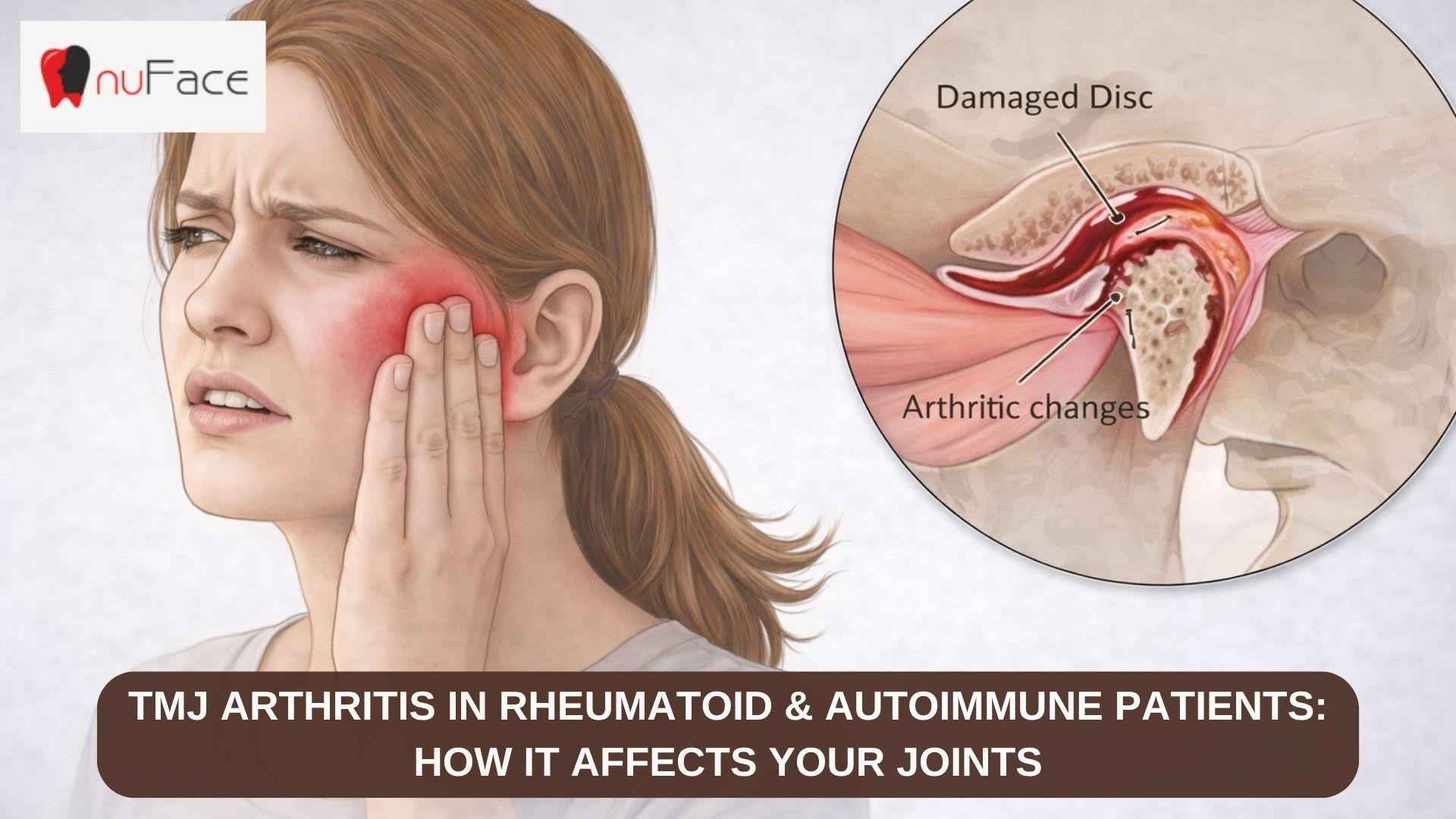
The temporomandibular joint, or TMJ, is the hinge that connects your jaw to your skull. You use it constantly. Chewing toast. Answering the phone. Muttering to yourself in traffic. So when rheumatoid arthritis or another autoimmune condition targets it, the impact sneaks into daily life in quiet but stubborn ways, explains Dr Nehal Patel, a TMJ specialist in India.
Why Autoimmune Diseases Target the Jaw
In rheumatoid arthritis, the immune system attacks the lining of joints. Not just the big obvious ones. Any synovial joint is fair game, and the TMJ qualifies. The tissue becomes inflamed, thickened, and painful. Over time, that inflammation can damage cartilage and bone.
TMJ arthroscopy specialists in India believe that autoimmune conditions like lupus, psoriatic arthritis, and juvenile idiopathic arthritis can affect the jaw too. Sometimes the TMJ symptoms appear years after diagnosis. Sometimes they show up first, which makes things confusing. A dentist might suspect grinding or stress. Meanwhile the real issue is happening deeper inside the joint.
If you wake up with jaw stiffness that slowly loosens as the day goes on, that pattern is suspicious. Morning stiffness is classic inflammatory arthritis behavior. Mechanical problems usually hurt more after heavy use, not before breakfast.
What TMJ Arthritis Actually Feels Like
It is not always dramatic pain. In fact, many people describe it as a dull ache near the ear, like you slept funny or chewed too much gum. There might be a sense of pressure or fullness. Some notice clicking or grinding sounds. Others just feel that their bite is “off,” as if the teeth no longer meet the way they used to.
During a flare, the joint can feel warm and tender to touch. Opening the mouth wide may be difficult, like the hinge is rusty. Eating something chewy such as groundnut or roasted corn suddenly becomes a strategic decision. You start cutting food into smaller pieces without really thinking about it.
TMJ Arthroscopy surgery specialists in India say headaches are common too. Not sharp migraines necessarily, but a steady tension around the temples or behind the eyes. Because the jaw muscles are working overtime to compensate, they tighten and complain.
Long Term Changes You Should Not Ignore
Here is the part that matters most. Chronic inflammation can slowly reshape the joint. The cartilage cushion thins, bone surfaces change, and movement becomes limited. In severe cases, the jaw can shift position, leading to bite changes or facial asymmetry.
For children and teens with autoimmune arthritis, TMJ involvement can even affect jaw growth. The lower jaw may not develop fully, which can alter facial structure over time. Adults do not face growth issues, but they can still experience progressive joint damage if inflammation stays uncontrolled.
Difficulty opening the mouth more than two fingers wide is a common warning sign. So is pain that does not improve with rest or standard TMJ remedies like mouthguards.
How It Affects Everyday Life
Jaw problems sound small until you live with them. Eating becomes slower. Conversations tire you out. Dental visits feel daunting because holding your mouth open hurts. Even brushing your teeth can trigger discomfort on bad days.
Sleep may suffer too. Some people clench in response to pain, which creates a vicious cycle. More clenching leads to more inflammation, which leads to more clenching. Not exactly restful.
Socially, it can be awkward. Declining chewy foods or avoiding long conversations makes people think you are distracted or uninterested. In reality, you are just trying not to aggravate your jaw.
When to Seek Help
If you already have an autoimmune diagnosis and develop persistent jaw symptoms, bring it up with your rheumatologist, who may point you to a TMJ specialist in India if required. Do not assume it is just stress or grinding. Imaging such as MRI can reveal inflammation long before X rays show damage.
Treatment usually focuses on controlling the underlying disease. Disease modifying medications, biologics, or targeted therapies often reduce TMJ inflammation along with symptoms elsewhere in the body. Dentists or oral medicine specialists may recommend physical therapy, gentle exercises, or custom splints to reduce strain.
Heat packs can soothe stiffness. Soft foods help during flares. And yes, sometimes simply giving your jaw permission to rest is the smartest move.
The Bottom Line
TMJ arthritis in autoimmune patients is easy to overlook but hard to live with. The jaw is small, yet its role in daily life is enormous. Pain here does not stay local. It affects how you eat, speak, sleep, and interact with the world.
If something feels persistently wrong, trust that instinct. Your jaw should not feel like a worn hinge every morning. Getting it checked early can prevent long term damage and make everyday tasks feel normal again. And honestly, being able to yawn without wincing is a small joy you do not appreciate until it is gone.